Root Canal Therapy in Windsor, Ontario
Save Your Natural Tooth & Relieve Pain
Why a Root Canal May Be Necessary
When the pulp (inner tissue) of a tooth becomes infected or inflamed, it can cause significant pain and lead to more severe oral health issues. Root canal therapy can:
✅ Eliminate infection and prevent further spread
✅ Relieve severe tooth pain and sensitivity
✅ Save your natural tooth from extraction
✅ Restore normal chewing and function
✅ Improve overall oral health
If left untreated, an infected tooth can lead to abscess formation, bone loss, or even systemic health issues. A timely root canal can help you avoid more extensive treatments.
Did you know?
- Root canals have a 95% success rate, making them one of the most effective dental treatments.
- Modern root canal therapy is virtually painless, thanks to advanced techniques and local anesthesia.
- Saving a natural tooth with a root canal helps maintain jawbone structure and prevents shifting of nearby teeth.
- A crown is usually placed after a root canal to strengthen and protect the treated tooth.
What to Expect During Root Canal Treatment
1️⃣ Thorough Examination & Diagnosis
We use digital X-rays to assess the affected tooth and confirm if a root canal is the best course of action.
2️⃣ Gentle Numbing & Infection Removal
Local anesthesia ensures a pain-free experience while we carefully remove the infected pulp and disinfect the tooth.
3️⃣ Filling & Sealing the Tooth
The cleaned tooth is filled with a biocompatible material and sealed to prevent reinfection.
4️⃣ Restoration with a Crown (If Needed)
A custom dental crown may be placed to restore strength, function, and appearance to the treated tooth.
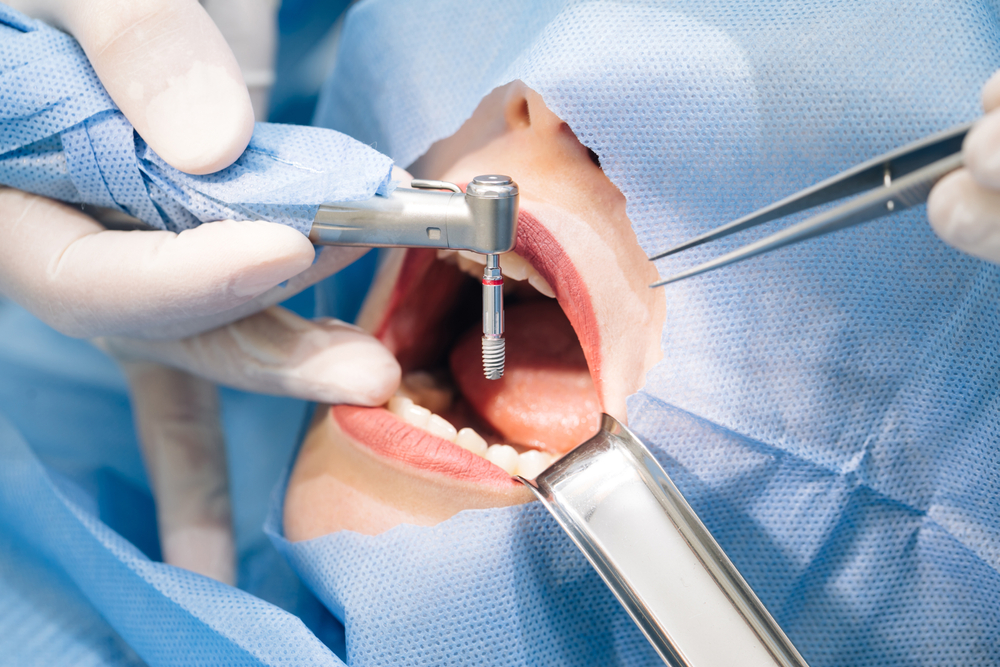
Frequently Asked Questions
Do root canals hurt?
Not at all! With modern anesthesia and techniques, root canals are as comfortable as getting a filling.
How long does a root canal take?
Most root canal treatments take one to two appointments, depending on the complexity of the case.
Will I need a crown after a root canal?
In most cases, yes—a dental crown helps reinforce the treated tooth, preventing fractures and ensuring long-term success.
How long does a root canal last?
A well-treated root canal can last a lifetime with good oral hygiene and regular dental checkups.
Don’t Let Tooth Pain Disrupt Your Life—Schedule Your Root Canal Today!
If you’re experiencing tooth pain or sensitivity, don’t wait—early treatment can save your tooth and prevent complications. Book an appointment with Walkerville Dental today!
